As COVID-19 cases continue to surge nationwide, healthcare workers at Stanford Health Care are speaking out about the toll the pandemic has taken on their mental health and their hopes surrounding vaccination.
“We were introduced to 2020 as the ‘Year of the Nurse,’ but none of us expected to be tested to this degree,” said nurse Diana Zhen.
Stanford Hospital is expected to reach record-high hospitalizations as an increasing number of COVID-19 patients are being admitted every day, according to emergency medicine doctor Ryan Ribeira. California’s governor recently issued a regional stay-at-home order in early December, requiring regions of the state to enact restrictions if their ICU capacity fell below 15%. Six counties in the Bay Area, including Santa Clara County, adopted the order before their ICU capacity dropped below the threshold in hopes of reducing COVID-19 cases and hospitalizations, but capacity fell to 12.9% as of Wednesday.
According to Santa Clara’s Department of Public Health, 96% of ICU beds were occupied with only 13 remaining as of Tuesday.
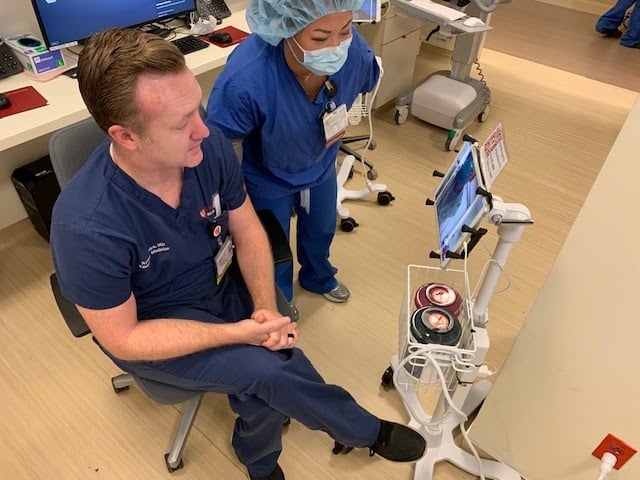
Concerned regarding the upcoming weeks, healthcare workers say they have been utilizing PPE and telemedicine, where iPads are used for supervision and communication between patients, their families and healthcare workers.
These protocols and safeguards “ensures only those needed at the bedside are at the bedside — never compromising patient care,” said emergency medicine doctor Laleh Gharahbaghian.
Earlier in the pandemic, doctors knew less about the virus and needed to adapt instantly. Healthcare workers described feeling anxious as they planned how to best assist COVID-19 patients while ensuring the safety of their other patients and coworkers.
There was “an immense sense of duty with pride in the ability to put my disaster training in emerging infectious diseases to work for the health and safety of our community,” Gharahbaghian told The Daily.
Nine months into the pandemic, doctors and nurses said they are still feeling that sense of duty, but added that they are experiencing high emotional stress and prolonged fatigue.
“It continues to be heart wrenching when sick patients must speak to their families over iPads, and our hands replace theirs when holding the patient’s hand,” Gharahbaghian said.
Healthcare workers feel “blessed” to have a supportive team along with the resources to help their patients, positive care doctor Dean Winslow told The Daily.
He added that he has been willing to work extra shifts, knowing that his younger colleagues have young children and are under an immense amount of stress. Like his colleagues, he carries a “sense of purpose” as healthcare workers strive for some sense of normalcy.
“I feel working on the wards at Stanford and caring for COVID-19 patients and other patients is a gratifying experience and it feels much the same way it did during my six combat deployments to Iraq and Afghanistan,” Winslow said.
The FDA recently approved a new COVID-19 vaccine manufactured by Pfizer on Dec. 11. The vaccine distribution has brought both hope and concerns for some healthcare workers as there are still uncertainties.
“The introduction of the vaccine is the first glimmer of hope we’ve received in this pandemic,” Zhen said.
This hope doesn’t come without anxieties, as studies have shown COVID-19 immunity may only last six to eight months, according to Ribeira. Because each person requires two doses of the vaccine and uncertainty persists regarding vaccine induced immunity, some healthcare workers are concerned about being able to provide the vaccine to 70% of the population to achieve herd immunity. Gharahbaghian also said she was concerned about the potential for mild vaccine side effects that could require healthcare workers to take time off.
During the vaccine distribution, nurse Sierra Kane explained the importance of continuing COVID-19 safeguards since there is still the possibility vaccinated individuals might be able to spread the virus.
With exhaustion setting in, healthcare workers are optimistic about the future. Despite fears, Winslow described the vaccine distribution as “a light at the end of the tunnel.”
Contact Alexandra Villanueva at tachis523 ‘at’ gmail.com.