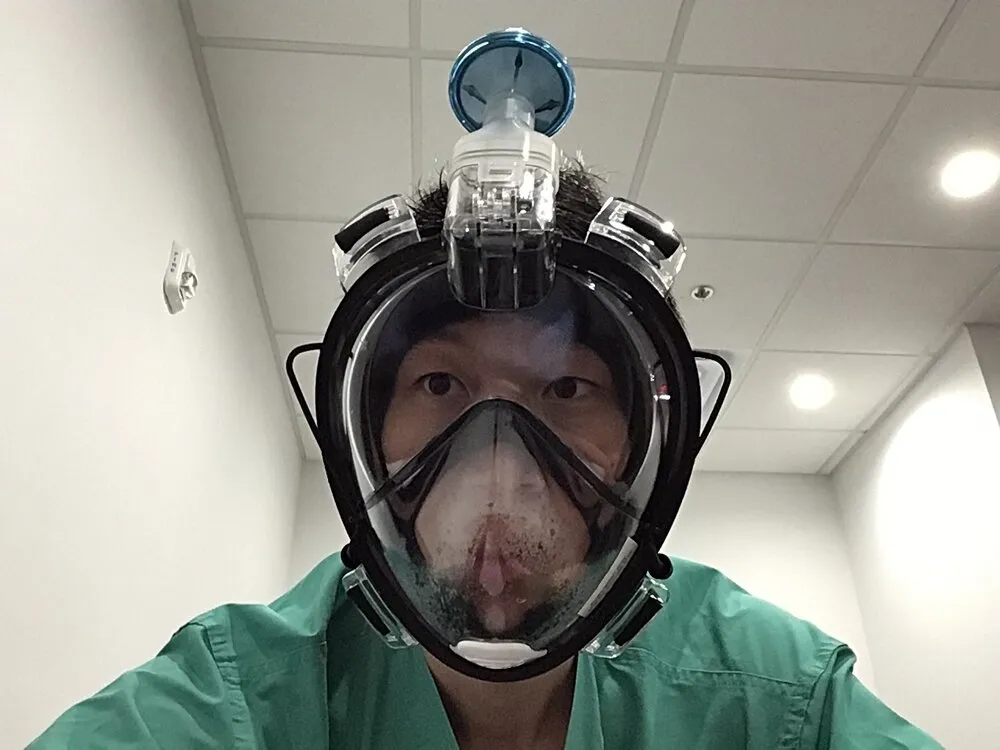
While stuck at home in March with old snorkeling gear from a past adventure, bioengineering professor Manu Prakash hypothesized that retrofitted snorkel masks might be able to serve as reusable and robust protective masks.
On April 29, the Prakash Lab and its collaborators released preliminary results of their reusable prototype: a snorkel mask whose snorkel has been replaced by 3D-printed adapters for a N95 filter cartridge.
Utilizing existing supply chains and partnerships, the team hopes to distribute tens of thousands of these snorkel-based “Pneumasks” to hospital systems across the country.
“There is a tremendous need for reusable masks in my community,” said Miami-based doctor Roberto Miki in a Pneumask testimonial. “The hospitals and other large groups have PPE and are able to absorb the elevated prices, but smaller practices like mine, which help cover emergent and urgent injuries, are left struggling to find and pay for PPE.”
According to the Pneumask website, 2,600 masks are already in use across the United States with agreements for thousands more to be financed and distributed in the coming days. The masks — designed specifically for medical frontline workers as opposed to general consumer use — fill an urgent need for high-quality reusable masks that doctors can both easily obtain and trust.
The project has required tremendous buy-in from graduate students and researchers.
Laurel Kroo, a sixth-year Ph.D. candidate in mechanical engineering in the Prakash Lab, dropped all work on completing her doctorate to help engineer Prakash’s snorkel idea.
“I remember feeling kind of down about my thesis one day and looking at the Slack channel and going, ‘That’s a really good idea,’” she said. “And Manu has like six of these ideas related to COVID. It’s exciting to work for a PI who can pivot the whole lab temporarily.”
Anesta Kothari, a researcher in the bioengineering department, said the team has worked on the project regularly “from around 8 a.m. to 12 a.m.” since mid-March.
“At the beginning we were looking at diagnostics as opposed to PPE gear, but soon we started looking at the other issues and very quickly began to work on Manu’s respirator idea,” Kothari said. “We started off pretty low key, just reverse engineering the connection kind of ad hoc and very quickly just to see whether or not it could work.”
Each mask consists of a full-face snorkel mask with the snorkel removed. Instead, an injection-molded coupler attaches to a medical-grade N95 filter. The three-part mask also comes with an alternate adapter for industrial-grade 3M filters. The masks are optimized for easy cleaning protocols and reusability, and they withstand many rounds of sterilization or filter replacement without any loss in safety.
On March 21, the lab shared its ideas in a public Google Doc.
“It wasn’t published or publicized or anything, just through our lab website,” Kothari said.
But the document blew up. Kothari and Kroo, whose Stanford emails were linked on the Google Doc, found their inboxes flooded with messages. Many of the emails came from clinicians, while others came from potential partners. One email came from medical-device company Boston Scientific, which immediately agreed to fund and distribute thousands of masks.
The close correspondence with clinicians and outside researchers helped to inform the team’s transparency and consistency in data collection and testing, evident in the eventual preprint article based on the original Google Doc.
“The mechanical design part of it is super easy compared to the testing and rigor behind the characterization, and I think that’s the main contribution that our lab has made,” Kroo said. “There are a lot of makers and groups out there, folks with 3D printers, sticking filters on masks. Our lab is saying: OK let’s look at CO2 levels, the filtration efficiency, the clinical usability, and starting off the discussions with the FDA.”
Many current custom masks are untrustworthy, as the seal to the face often degrades long before filters actually wear out. The snorkel mask removes these problems, but there are still fit issues for people with large beards or glasses. Many hospital personnel have already shaved their beards or switched to contact lenses.
The masks are currently FDA-approved as face shields, but they are awaiting approval as respirators. But while partner organizations such as Boston Scientific have agreed to fund batches of thousands of the masks for immediate distribution to hospitals, the largest barrier to further adoption is the cost of the masks. In North America, most of the snorkel masks have to be purchased at full market price, which can run around thirty dollars each.
In France, the pen company BIC has manufactured 25,000 free Pneumasks using their existing factory infrastructure and agreed to perform further injection molding to ensure extremely high tolerances.
The Pneumask is the most developed of the Prakash Lab’s current projects, but there are others.
One of the most ambitious is Project 1000 x 1000, which aims to use a “cotton candy machine” approach to spin styrofoam into a nano-fiber electrostatically charged N95-grade filter material. If a thousand small businesses were to build the Project 1000 by 1000 system, which only requires spinning tools such as a Dremel available at any hardware store, they could each produce thousands of masks every day, the lab says. The “cotton candy machine” concept is the brainchild of Anton Molina, a current Ph.D. candidate in materials science.
The Prakash lab prioritizes cheapness and scale in an approach known as “frugal science.” It is known for its Foldscope, a dirt-cheap microscope for science education, but has ventured into medical technology before with tools like Paperfuge, a low-cost centrifuge, and MalariaScope, a smartphone attachment that can analyze blood smears to determine someone’s probability of having malaria. Its current ventilator projects are designed for the third world, aimed to minimize health worker labor needs or general cost of parts.
Contact Cooper Veit at cveit ‘at’ stanford.edu.