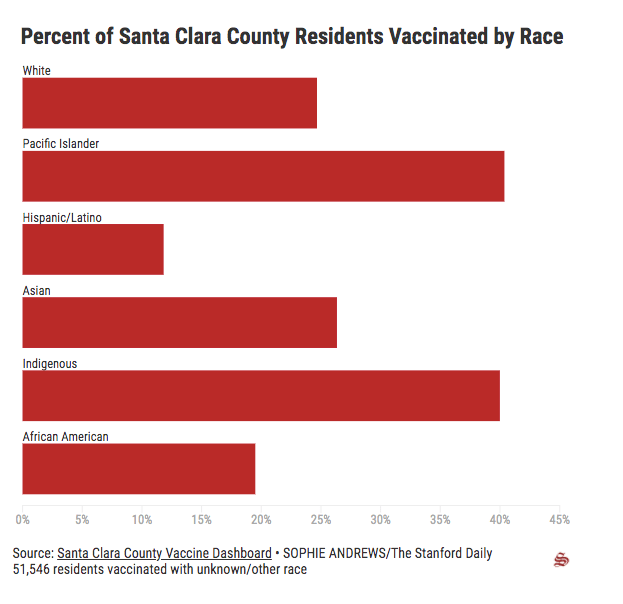
Black and Latinx residents in Santa Clara County (SCC) are being vaccinated at lower rates than white and Asian residents, according to the county vaccine dashboard.
Only 11.82% of Hispanic/Latino residents and 19.5% of African-American residents aged 16 and older have been vaccinated. SCC’s two largest racial demographics are white and Asian, and approximately a quarter of each of these groups has been vaccinated.
Stanford Health Care Chief of Staff Megan Mahoney said these racial disparities are especially concerning because Latinx and African-American populations have been disproportionately affected by COVID-19. According to the county’s COVID demographic data, the Latinx community constitutes 25.8% of the population but make up 50.9% of COVID-19 cases.
In total, 25.5% of SCC residents aged 16 and older have received their first dose of the vaccine, and 13.7% have received both doses as of Tuesday, according to the dashboard. Workers in education and childcare, emergency services and agriculture and food are the newest groups being vaccinated, joining healthcare workers and those over 65.
Stanford researchers said financial, cultural, transportation and trust barriers could be the reasons for these disparities in vaccination rates.
According to medicine professor Dean Winslow, many members of the Latinx community work minimum wage jobs and may have poor health insurance and lack healthcare access, creating challenges for them to get their vaccines.
Some members of the Latinx community are also undocumented, and there could be some fear of “showing up publicly and receiving the vaccine,” Winslow said.
Though vaccine trust is currently at an “upswing,” according to pediatrics professor Grace Lee, there are still significant differences by race and ethnicity –– another possible cause of the inequity in vaccination rates.
Epidemiology and population health assistant professor Lisa Goldman Rosas wrote in an email to The Daily that historical and recent injustices have caused higher levels of mistrust among African-American and Latinx communities.
However, citing a New York Times op-ed by pediatrics adjunct clinical instructor Rhea Boyd, Mahoney said, Boyd “states that the concept of vaccine hesitancy implicitly blames African Americans, where the issue is more likely to be vaccine access and not hesitancy.”
These access barriers include geographical location and transportation challenges, according to Mahoney and Winslow. Poor mass transit systems could impede access to vaccine appointments and sites, Winslow added.
Additionally, Mahoney said language barriers also exist, contributing to the gap in people’s access to vaccine information and affecting their ability to make informed decisions about receiving the vaccine.
In response, the county is expanding its COVID-19 paid advertising campaign to include “English, Spanish, Vietnamese, Chinese and Tagalog across multiple platforms, including local television, television stations and locally zoned cable channels,” according to manager of the county’s Office of Labor Standards Enforcement Betty Duong in a Board of Supervisors meeting on March 10.
The county also has a data-driven vaccine equity plan, determining priority groups based on census tracts that consider factors such as vaccination rates, COVID-19 positivity rates and share of Latinx residents. This data helps the county decide where to send outreach teams and set up mobile vaccine clinics, according to Office of the County Executive program manager Brian Darrow.
It is crucial for healthcare systems to set up clinics and neighborhood-based vaccination sites in areas that may lack access to large health centers and face low vaccine coverage, Lee said. Having staff that are culturally and linguistically competent is also key, according to Goldman Rosas.
“It’s really going to be about ensuring that the voices of those communities are reflected in the conversations about both efficacy and safety of the vaccine,” Lee said.
Recently, the county has aided in setting up clinics at Emmanuel Baptist Church, Gilroy High School, East Valley Clinic and Eastridge Mall, which Stanford Health Care (SHC) is operating.
“Government, medical and public health institutions bear the responsibility of increasing their trustworthiness,” Goldman Rosas said. “This is different than placing the responsibility on communities to increase their trust.”
To address this, the county has turned toward community outreach, partnering with community health workers and local leaders that understand their communities.
According to Mahoney, SHC provided volunteers to Ravenswood Health Center in East Palo Alto during a February vaccination event, which led to over a thousand patients being vaccinated.
Deputy County Executive of the SCC Public Health Department (SCCPHD) Rocio Luna said during the Board of Supervisors meeting that the SCCPHD has partnered with the fire department to address the existing vaccine gaps.
“The public health department will focus primarily on the 52 skilled nursing facilities, while County Fire will focus on long term care facilities and in-home vaccine delivery,” Luna said.
Meanwhile, the county’s Groundworks Campaign is doing door-to-door residential outreach to provide vaccine education and eventually vaccine scheduling, according to Darrow.
The county has also created a priority appointment slot system that community partners and outreach teams can use to schedule appointments, which has been effective in improving vaccine access for hard-hit communities: more than a thousand of the over 1,800 appointments that were scheduled were Latinx residents, Darrow said.
“We’re making progress, although … until we get closer to probably 75 or 80% of the population immunized, we’re still going to have to be careful about continuing to follow the physical mitigating measures that we use to reduce transmission,” Winslow said.