The microfluidic guillotine, a new cell cutting device developed by Stanford scientists, revolutionizes the process of dividing individual cells for research. The new device opens doors for medical research on cell repair to reduce the implications of cancer and degenerative diseases.
For the past century, scientists have used glass needles to cut cells under a microscope. The first cells would have partially healed by the time the hundredth cell was cut. Assistant professor of mechanical engineering Sindy Tang M.S. ’04 and her lab developed the microfluidic guillotine to speed up the cutting process up to 64 cells each minute.
“Instead of moving the knife against an immobile cell, we would be moving the cell against a knife that is fixed, so kind of like a sausage cutter,” Tang said. “That idea was there from pretty early on.”

The group used polydimethylsiloxane (PDMS), a substance that can be alternatingly viscous or elastic depending on conditions, making it common in microfluidic devices. According to Lucas Blauch M.S. ’16 Ph.D. ’19, head researcher on the study, PDMS is well-developed and precise for cutting cells.
“So at first we tried crazy things,” Blauch said. “We tried using wires to cut the cell. I really wanted to try to use my hair to cut the cell, but at the end of the day those weren’t as precise.”
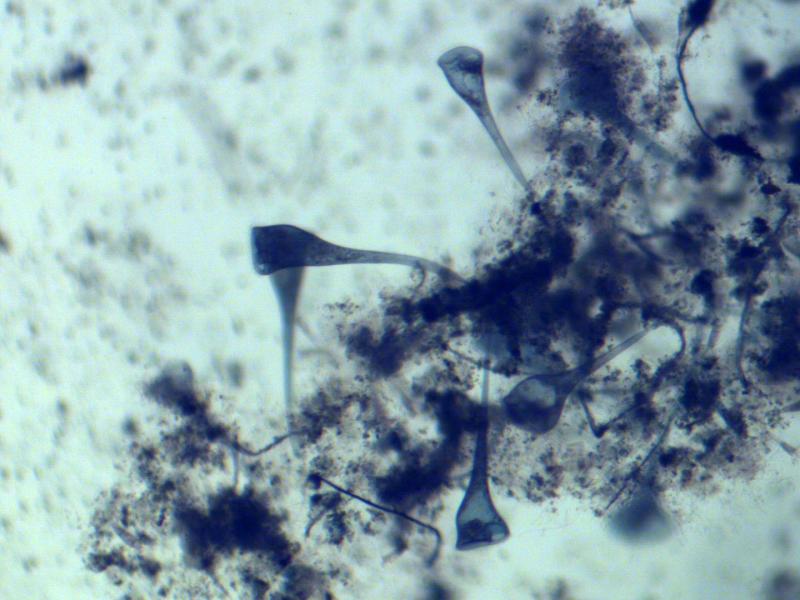
Tang developed the idea for the device while studying single-cell repair in Stentor coeruleus, a one-millimeter long ciliate protist resembling a trumpet. According to Tang, Stentor’s extensive healing properties make it ideal for studying how individual cells regenerate after being wounded.
According to a paper Tang and Blauch co-authored, the guillotine will be used to synchronize studies on wound repair. Although there are many studies showing the properties of multicellular organism cell-repair, there are fewer studies on the healing properties of individual cells. The guillotine’s rapid bisection allows researchers to look at each cell fragment accurately.
Understanding cell repair aids medical research about healing cells in degenerative diseases that prevent cell replication, such as in muscular dystrophy, myocardial infarction and neurodegenerative diseases. The same concept also applies to preventing cell repair in cancer.
“We’re hoping to learn about ways to either prevent or enhance single cell wound healing depending on the desired effect for the disease,” Blauch said.
Contact Jessica Jen at jessicajen23 ‘at’ gmail.com